![Blood Sugar and Diabetes on a Plant-Based Diet: The Reversal Evidence [2026]](https://makeitplantbased.com/images/articles/blood-sugar-diabetes-plant-based-diet/blood-sugar-diabetes-plant-based-diet-featured.webp)
If someone told you that eating more carbohydrates could reverse type 2 diabetes, you’d probably think they were joking. In a world where low-carb and keto diets dominate the diabetes conversation, the idea that a high-carb, whole-food plant-based diet could achieve what medications often cannot sounds counterintuitive. Yet that’s exactly what the research shows — and it’s what leading WFPB doctors have been demonstrating in their clinical practices for decades.
The key insight is that not all carbohydrates are the same. Whole plant foods — beans, whole grains, fruits, and vegetables — come packaged with fiber, resistant starch, and phytochemicals that actually improve insulin sensitivity. It’s the refined carbohydrates and dietary fat that drive insulin resistance, not carbohydrates from whole plants. This guide examines the research, the doctor protocols, and the practical steps for using a plant-based diet to take control of blood sugar.
How Insulin Resistance Actually Works: The Fat-Sugar Connection
Insulin resistance is often misunderstood as a “carbohydrate problem.” In reality, the primary driver is intramyocellular lipid accumulation — fat buildup inside muscle cells that interferes with insulin signaling. When fat accumulates inside cells that aren’t designed to store it (muscle cells, liver cells), it disrupts the insulin receptor’s ability to respond to insulin. The result: glucose can’t enter the cells efficiently, and blood sugar rises.
This is why a whole-food, plant-based diet works so well for insulin sensitivity: it’s naturally low in saturated fat, which is the type most associated with intramyocellular lipid buildup. By reducing dietary saturated fat and increasing fiber intake, plant-based diets address the root cause of insulin resistance rather than just managing blood sugar through carb restriction.
Fiber: The Unsung Hero
Dietary fiber slows carbohydrate absorption, prevents blood sugar spikes, and feeds beneficial gut bacteria that produce short-chain fatty acids involved in glucose metabolism. The average plant-based eater consumes 40-50 grams of fiber daily compared to 15-17 grams on a standard American diet. This difference alone has profound effects on blood sugar control.

The High-Carb Myth Debunked: Why Whole Plant Carbs Improve Blood Sugar
Low-carb diets improve blood sugar numbers in the short term by removing the substrate (carbohydrates) that becomes glucose. But they don’t address the underlying insulin resistance — they work around it. When someone on a keto diet eats a carb-rich meal, their blood sugar spikes even higher than before because their insulin resistance hasn’t improved.
A whole-food, plant-based diet takes the opposite approach: it improves insulin sensitivity itself, so the body can handle carbohydrates properly. A 2021 perspective published in Advances in Nutrition outlined the mechanisms by which plant-based eating prevents and treats type 2 diabetes — including reduced intramyocellular lipids, improved beta-cell function, and favorable changes in gut microbiota.
Research and Statistics: The Diabetes Reversal Evidence
The evidence for plant-based diets and diabetes management is among the strongest in nutrition science:
A 2024 randomized controlled trial of a whole-food, plant-based intensive lifestyle intervention found significant improvements in glycemic control, with participants able to reduce their diabetes medications. This was achieved while eating a high-carbohydrate diet — demonstrating that carbohydrate quality matters more than carbohydrate quantity.
A 2024 case series documented remission of type 2 diabetes after treatment with a high-fiber, low-fat, plant-predominant diet. Patients achieved normal blood sugar levels and came off diabetes medications entirely.
A 2024 systematic review and meta-analysis of RCTs on vegetarian and vegan dietary patterns for type 2 diabetes confirmed significant improvements in HbA1c, fasting glucose, and body weight compared to conventional diabetes diets.

What Plant-Based Doctors Say About Diabetes and Blood Sugar
Dr. Neal Barnard
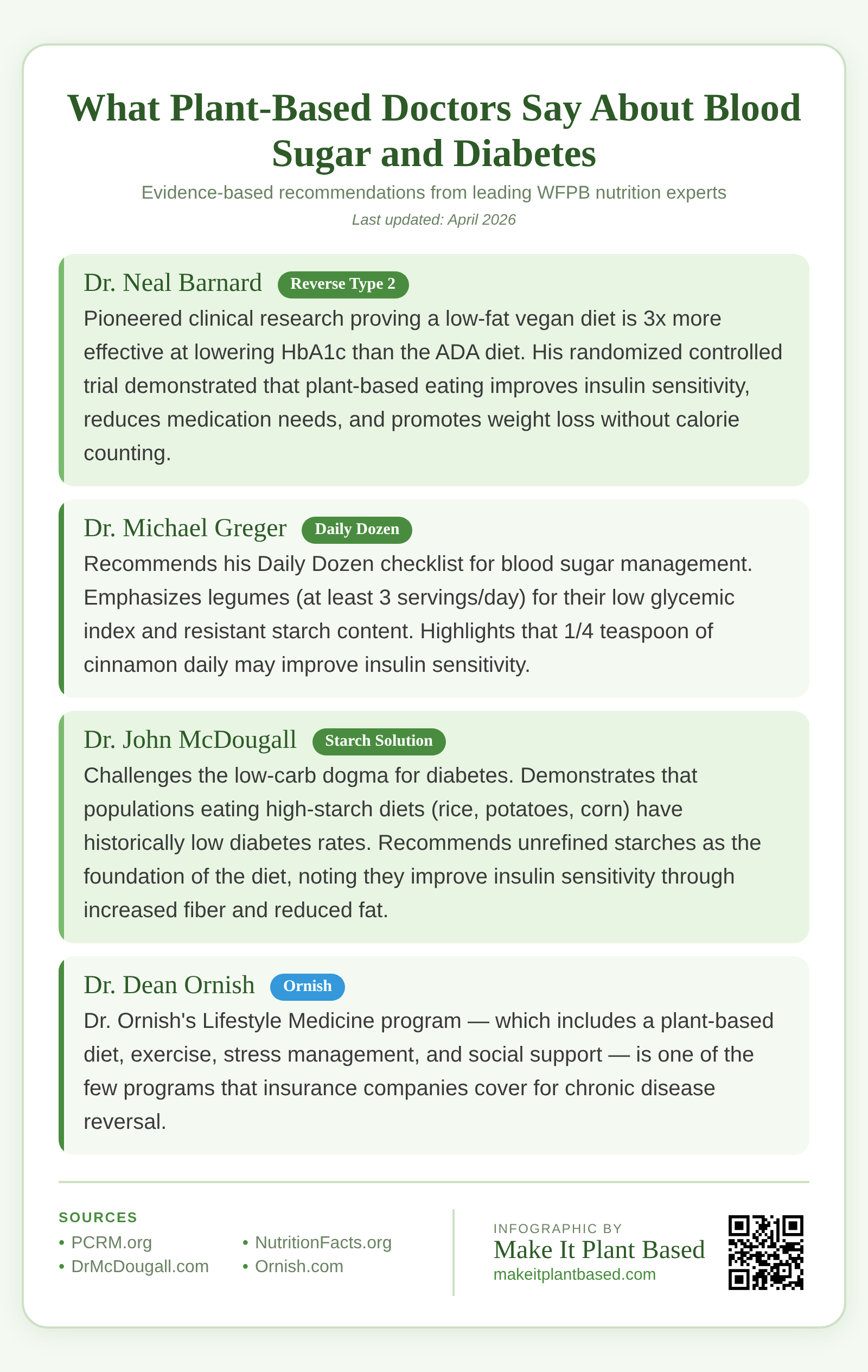
Dr. Barnard has conducted groundbreaking clinical trials on plant-based diets for diabetes. His research, published in peer-reviewed journals, demonstrated that a low-fat vegan diet improved glycemic control three times more effectively than the American Diabetes Association’s standard dietary recommendations. His protocol emphasizes a low-fat, plant-based diet with no calorie counting required — the high fiber and low caloric density naturally regulate portion sizes. PCRM’s diabetes program has helped thousands of patients reduce or eliminate diabetes medications. (PCRM — Diabetes Program)
Dr. Michael Greger
Dr. Greger has extensively covered the diabetes reversal evidence on NutritionFacts.org. He emphasizes the intramyocellular lipid mechanism — how dietary fat (particularly saturated fat) causes fat buildup inside muscle cells, which is the root cause of insulin resistance. He highlights that whole-food plant-based diets resolve this by being naturally low in saturated fat. He also covers the role of specific foods: beans and lentils for blood sugar stabilization, turmeric for reducing inflammation in pancreatic beta cells, and vinegar for blunting post-meal glucose spikes. (NutritionFacts.org — Reverse Type 2 Diabetes)
Dr. John McDougall
Dr. McDougall’s starch-based approach directly challenges the low-carb paradigm for diabetes. He argues that rice, potatoes, corn, and beans are the foods that have sustained healthy populations for millennia, and that diabetes is caused by the fat and refined foods of the Western diet, not by starch. His residential programs have documented dramatic blood sugar improvements in participants who switch to a starch-based diet — often seeing fasting glucose drop within days of the dietary change.
Dr. Dean Ornish
Dr. Ornish’s Lifestyle Medicine program — which includes a plant-based diet, exercise, stress management, and social support — is one of the few programs that insurance companies cover for chronic disease reversal. His research has shown improvements in insulin sensitivity, weight loss, and cardiovascular risk factors in diabetic patients. The comprehensive approach addresses the lifestyle factors that drive metabolic syndrome. (Ornish Lifestyle Medicine)
Type 2 Diabetes Reversal: What “Reversal” Really Means
When doctors talk about “reversing” type 2 diabetes with diet, they mean achieving and maintaining normal blood sugar levels (HbA1c below 6.5%) without diabetes medications. This doesn’t mean the underlying genetic susceptibility disappears — it means the metabolic dysfunction has been corrected through dietary and lifestyle changes.
The evidence shows that 23-37% of participants in plant-based diet interventions achieve full diabetes remission, and the majority experience significant improvements in blood sugar control and medication reduction even if they don’t achieve full remission. These are remarkable results for a dietary intervention with no side effects.
Practical Meal Planning for Blood Sugar Control
Focus on legumes: Beans, lentils, and chickpeas have the lowest glycemic index of any starchy food. They’re also rich in resistant starch, which feeds beneficial gut bacteria. Aim for at least 1-2 cups of legumes daily.
Choose intact whole grains: Steel-cut oats, brown rice, quinoa, and barley have much lower glycemic impact than refined grains. The intact grain structure slows digestion and prevents blood sugar spikes.
Load up on non-starchy vegetables: Leafy greens, broccoli, peppers, and cruciferous vegetables provide nutrients and fiber with minimal blood sugar impact. Aim for half your plate to be non-starchy vegetables.
Minimize added oils: Even “healthy” oils are pure fat and contribute to the intramyocellular lipid accumulation that drives insulin resistance. Cook with water, vegetable broth, or small amounts of whole food fats (avocado, nuts).

Type 1 Diabetes Considerations
While type 2 diabetes is driven by insulin resistance, type 1 diabetes is an autoimmune condition where the pancreas doesn’t produce insulin. Plant-based diets can still benefit type 1 diabetics: a 2024 randomized clinical trial found that a plant-based dietary intervention reduced insulin requirements by 28% in type 1 diabetic patients over 12 weeks, while also improving glycemic control. The mechanism is improved insulin sensitivity, which means each unit of injected insulin works more effectively.
Key Research References
- 2021 perspective: plant-based eating for type 2 diabetes prevention and treatment
- 2024 RCT: whole-food plant-based intervention improves glycemic control
- 2024 case series: type 2 diabetes remission on a plant-predominant diet
- 2024 systematic review and meta-analysis: vegan diets for type 2 diabetes
- 2024 RCT: plant-based diet reduces insulin requirements in type 1 diabetes
Frequently Asked Questions About Blood Sugar and Plant-Based Diets
Can a plant-based diet reverse type 2 diabetes?
Yes. Clinical studies show that 23-37% of participants achieve full diabetes remission on a whole-food, plant-based diet, and the majority experience significant improvements in blood sugar control and medication reduction.
Is a high-carb vegan diet safe for diabetics?
When the carbohydrates come from whole plant foods (beans, whole grains, fruits, vegetables), yes. These foods are high in fiber and resistant starch, which slow glucose absorption and improve insulin sensitivity — the opposite of refined carbs.
How quickly can a plant-based diet improve blood sugar?
Many people see improvements in fasting blood sugar within days to weeks of switching to a whole-food plant-based diet. Significant HbA1c improvements typically appear within 3-6 months, with some achieving medication reduction within weeks under medical supervision.
What is the best plant-based diet for diabetes management?
A low-fat, whole-food, plant-based diet centered on legumes, whole grains, vegetables, and fruits — minimizing added oils and processed foods. Dr. Barnard’s protocol and Dr. McDougall’s starch-based approach have the most clinical evidence.
Can you come off diabetes medication with a plant-based diet?
Many people do, but this must be done under medical supervision. As blood sugar improves, medication doses need to be adjusted to avoid hypoglycemia. Work closely with your healthcare provider when making dietary changes.
Does a plant-based diet help with type 1 diabetes?
A 2024 clinical trial showed a 28% reduction in insulin requirements for type 1 diabetics on a plant-based diet. The improved insulin sensitivity means each unit of injected insulin is more effective.
The Fiber Advantage: How Plant Foods Slow Glucose Absorption
The primary mechanism by which plant-based diets prevent and reverse type 2 diabetes is through fiber’s profound effect on glucose absorption. Dietary fiber, found exclusively in plant foods, physically impedes carbohydrate digestion and glucose absorption in the small intestine. Soluble fiber from oats, legumes, and pectin-rich fruits forms a viscous gel that slows food movement through the digestive tract, creating a more gradual glucose rise rather than the sharp spikes that challenge insulin production. Insoluble fiber from whole grains and vegetables adds bulk and alters transit time, further moderating glucose absorption patterns. This flattening of the blood glucose curve is not merely a temporary effect—it represents a fundamental shift in how the body processes carbohydrates.
Resistant Starch and Blood Sugar Control
Resistant starch, a specific type of carbohydrate found abundantly in cooked and cooled legumes and certain whole grains, behaves more like fiber than digestible carbohydrate. When legumes like beans and lentils are cooked and cooled, their starch structure transforms into resistant starch, which escapes digestion in the small intestine and reaches the colon intact. Rather than raising blood glucose, resistant starch feeds beneficial gut bacteria and produces short-chain fatty acids that improve metabolic health. Research shows that meals incorporating resistant starch cause substantially lower blood glucose and insulin responses compared to equivalent meals with regular digestible starch. This mechanism explains why bean-based diets show such dramatic blood sugar improvements.
The Gut Microbiome Connection
Recent research reveals that the gut microbiome is central to diabetes prevention and reversal. Plant-based diets, with their high diversity of fiber sources and plant compounds, dramatically reshape the gut bacterial ecosystem. The abundant plant fiber selectively feeds beneficial bacteria that produce short-chain fatty acids (SCFAs), particularly butyrate. These SCFAs perform multiple anti-diabetic functions: they strengthen the intestinal barrier preventing endotoxin translocation, reduce systemic inflammation, improve insulin sensitivity in muscle and liver, and enhance satiety signaling. Studies comparing omnivorous and plant-based individuals show dramatically different bacterial compositions, with plant-based individuals having microbial communities that produce significantly more butyrate and have reduced pathogenic bacteria associated with metabolic dysfunction.
Weight Management and Diabetes Prevention
Plant-based diets support healthy weight maintenance through their inherently lower caloric density. Because plant foods are fiber-rich and water-rich while relatively low in calories, people can eat satisfying food volumes while consuming fewer calories than on omnivorous diets. A 2000-calorie diet based on whole plant foods provides substantially more food volume and satiety than 2000 calories from calorie-dense animal products and processed foods. The increased satiety from fiber and water content reduces overeating and supports natural, effortless weight loss. Since excess weight is a primary driver of insulin resistance and type 2 diabetes, this weight management benefit represents a crucial mechanism of disease prevention. Research consistently shows that plant-based dieters achieve and maintain lower body weights compared to omnivorous controls.
Superfoods for Blood Sugar Management
Certain plant foods have demonstrated particularly strong effects on blood sugar control. Cinnamon contains compounds that improve glucose utilization and enhance insulin secretion; studies show that just ½ teaspoon daily improves fasting glucose levels. Turmeric’s curcumin reduces inflammation and improves insulin sensitivity through multiple molecular pathways. Bitter melon contains compounds that mimic insulin and increase glucose uptake; traditional use in Asian medicine is now validated by clinical research. Fenugreek seeds contain soluble fiber and compounds that slow glucose absorption and improve insulin response. Incorporating these foods into a plant-based diet creates a synergistic effect where multiple mechanisms simultaneously support blood sugar control.
Type 1 Diabetes: Plant-Based Support for Blood Sugar Management
While type 1 diabetes is an autoimmune condition not preventable through diet alone, plant-based eating offers significant advantages for blood sugar management in type 1 diabetes. Because plant-based diets provide more stable, gradual glucose absorption patterns, individuals with type 1 diabetes experience less dramatic blood glucose fluctuations and require more moderate, predictable insulin dosing. The high fiber content reduces postprandial glucose peaks, meaning smaller insulin injections are needed after meals. Additionally, the anti-inflammatory nature of plant-based eating may help preserve remaining beta cell function and reduce immune activation against pancreatic cells. Many type 1 diabetics following plant-based diets report improved glycemic control, reduced glucose variability, and better quality of life compared to omnivorous eating patterns.
Take the guesswork out of plant-based nutrition.
Explore our evidence-based guides on the nutrients that matter most.
Browse All Nutrient Guides